| Journal of Clinical Gynecology and Obstetrics, ISSN 1927-1271 print, 1927-128X online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Clin Gynecol Obstet and Elmer Press Inc |
| Journal website http://www.jcgo.org |
Case Report
Volume 4, Number 1, March 2015, pages 188-190
Recurrent Ectopic Pregnancy Following Ipsilateral Proximal Salpingectomy
Shamma Al-Inizi
Department of Obstetrics and Gynaecology, South Tyneside NHS Foundation Trust, NE340PL, UK
Manuscript accepted for publication February 23, 2015
Short title: Recurrent Ectopic Pregnancy
doi: http://dx.doi.org/10.14740/jcgo313w
| Abstract | ▴Top |
Ectopic pregnancies are pregnancies implanted outside the uterine cavity and reported approximately to affect 1 in 100 pregnancies, most commonly occurring in the fallopian tubes. It is very rare for the ectopic pregnancy to recur in the distal remaining portion of the ipsilateral fallopian tube following proximal salpingectomy. We are reporting a 27-year-old nulliparous lady with previous right proximal salpingectomy for ectopic pregnancy presenting with recurrent ipsilateral distal tubal ectopic pregnancy and was managed surgically. Despite it is very rare, ectopic pregnancy can recur in the distal remaining part of a fallopian tube following proximal salpingectomy. Whenever the tubal ectopic pregnancy is managed surgically, we recommend performing total salpingectomy to avoid this occurrence.
Keywords: Ectopic pregnancy; Recurrent; Salpingectomy
| Introduction | ▴Top |
Ectopic pregnancy presents a major health problem for women of childbearing age. It is the result of a flaw in human reproductive physiology that allows the conceptus to implant and mature outside of the endometrial cavity, which ultimately ends in the demise of the fetus. Without timely diagnosis and treatment, ectopic pregnancy can become a life-threatening situation.
Ectopic pregnancy causes major maternal morbidity and mortality with pregnancy loss, and its incidence is increasing worldwide. A history of pelvic inflammatory disease is particularly important and has been implicated in the increased incidence of ectopic pregnancy. Recurrent ectopic pregnancy is a more serious issue especially when it occurs in the remnant part of a fallopian tube which was thought to have been removed in a previous tubal ectopic pregnancy operation. High index of suspicion and appropriate investigations should lead to the best management plan.
| Case Report | ▴Top |
A 27-year-old nulliparous lady presented with a history of 6 weeks amenorrhoea, right-sided pelvic pain and mild vaginal bleeding. She had stable vital signs and a hemoglobin level of 11 g/dL. She had previous right-sided proximal partial salpingectomy for ectopic pregnancy 10 years ago which has been confirmed by histology. Previous operative notes indicated some degree of difficulty during previous right salpingectomy necessitating sparing the distal end of the right fallopian tube due to bowel adhesions. Pelvic ultrasound scan indicated an empty uterus with some intra-abdominal bleeding. She had a β-hCG level of 4,740 IU. A decision to perform a laparoscopy was taken.
At laparoscopy, there was a normal left fallopian tube and a 3 × 2 cm right-sided ectopic tubal mass adherent to the large bowels and the mass was bleeding. There was around 400 mL of blood in the peritoneal cavity (Fig. 1). There were per-hepatic adhesions indicating previous chlamydial infection (Fig. 2). The proximal end of the right fallopian tube was absent indicating previous right proximal salpingectomy. The tubal mass was dissected from the bowels and distal salpingectomy was performed. Tubal pregnancy was confirmed on histology. The patient made good post-operative recovery and was discharged next day in good condition.
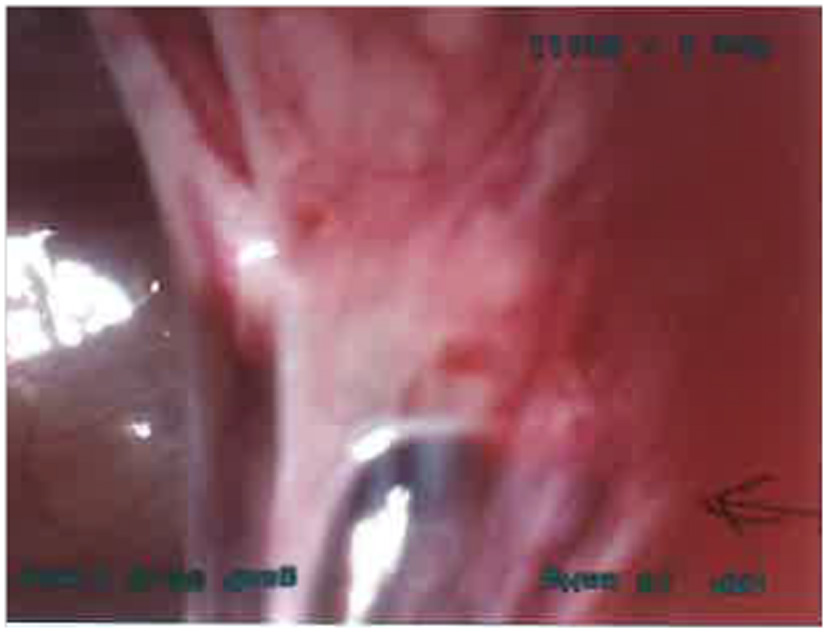 Click for large image | Figure 1. The ectopic pregnancy mass adherent to large bowels. |
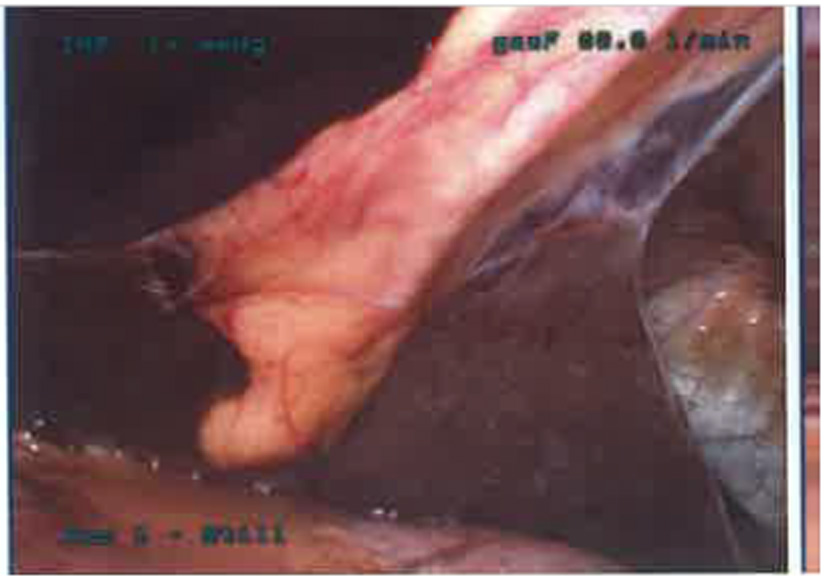 Click for large image | Figure 2. Peri-hepatic adhesions (Fitz-Hugh). |
| Discussion | ▴Top |
Ectopic pregnancy remains the leading cause of pregnancy-related first trimester deaths worldwide [1].
The incidence of recurrent ectopic pregnancy is approximately 15% which rises to 30% following two previous ectopic pregnancies [2, 3].
Recurrent ectopic pregnancy occurring in the proximal remaining stump of the tube following ipsilateral distal salpingectomy has been reported before [3, 4].
The incidence of ectopic pregnancy has increased markedly over the last three decades. This is probably due to multiple factors such as the increased prevalence of pelvic inflammatory disease, use of assisted reproductive technology, increasing maternal age and earlier more accurate diagnosis [4, 5]. One ectopic pregnancy is a risk factor for another ectopic pregnancy. Contralateral ectopic pregnancy following salpingectomy is not uncommon occurring in around 15% of pregnancies [3, 6]. Diagnosis of ectopic pregnancy is usually based on a combination of clinical suspicion in conjunction with ultrasonographic findings and suboptimal rise in serial serum human chorionic gonadotropin beta subunit (β-hCG) with no intrauterine pregnancy demonstrated on pelvic ultrasound scan.
Ipsilateral ectopic pregnancy following salpingectomy is rare, with very few cases reported in the English literature in the last 10 years [7]. This particular type of ectopic pregnancy is associated with mortality rates 10 - 15 times higher than other ectopic pregnancies [8]. Recurrent ectopic pregnancy in the proximal remnant of the ipsilateral fallopian tube following previous distal salpingectomy has been reported previously [4]. This could be explained by the hypotheses of spermatozoa passing through the patent tube, into the Pouch of Douglas, and travel to fertilize the ovum on the side of the damaged tube which then is picked up by the remaining tubal stump [9]. Another hypothesis is that an oocyte from the contralateral ovary might have been fertilized normally in the patent tube and then later implanted in the stump via intrauterine migration [10]. Another hypothesis is that despite the ligation of the tube following salpingectomy, some degree of patency or recanalization may occur. This thus provides a communication between the endometrial and peritoneal cavities and allows for fertilization and implantation within the isthmic portion of the remnant tube [7]. The use of endo loop ligation for the surgical treatment of ectopic pregnancy has been considered to result in ipsilateral ectopic pregnancy in the remaining tubal stump [7].
Recurrent ectopic pregnancy in the distal remaining end of a fallopian tube following ipsilateral proximal salpingectomy is very rare. The MEDLINE was searched for similar cases and only one case was reported in the literature [6].
There are two possible postulations behind the occurrence of distal ipsilateral ectopic pregnancy following proximal salpingectomy. The first is the passage of spermatozoa or the fertilized egg from the intact fallopian tube through the pouch of Douglas to the contralateral tubal remnant. Secondly, the lumina persists in the interstitial portion of the remaining tube and the distal tubal remnant allowing communication between the endometrial cavity and the distal tubal remnant which facilitates the passage of sperms or fertilized egg to the distal tubal remnant. In this case, the first hypothesis applies as intra-operatively the distal remnant of the tube was adherent to bowels and separate from the proximal tubal stump and uterus.
Theoretically, total salpingectomy eliminates the risk of an ipsilateral tubal pregnancy. However, total salpingectomy is difficult to achieve using endoloops alone. However, it can be achieved using diathermy, harmonic or ligasure scalpels.
Cases that leave a tubal remnant behind may well need to be considered as akin to salpingostomy in terms of the risk of ectopic pregnancy recurrence. Whilst few generalizations can ever be made from a case report, it is important for clinicians to be aware of this inherent problem, especially as it is not the only consequence. Hydrosalpinges can develop in tubal stumps, resulting in decreased fertility by interfering with implantation and pelvic anatomy needing further surgical intervention. This is usually when the proximal tubal remnant is left. However, leaving the distal remnant can still lead to recurrent ectopic pregnancy despite it is rare, which has been presented in this case.
Given the uncertain nature of the mechanism of ipsilateral recurrent ectopic pregnancy in the tubal remnant, selecting a method for prevention is difficult. However, a few options may be suggested to decrease the probability of recurrence. When performing the salpingectomy, care should be taken not to leave a long tubal stump remaining [4]. It should be noted that, generally, it is common practice to leave a long tubal stump to minimize the risk of bleeding associated with the isthmic portion of the fallopian tube. However, given the risk of future ectopic pregnancies in those with a history of ectopic pregnancy, it may be suggested that this remnant portion should be minimized and trial to remove the whole tube including the distal end even if it is adherent to the bowels to prevent recurrence of the ectopic pregnancy in that remnant should always be the case.
Conclusion
Recurrent ectopic pregnancy in the distal tubal remnant following ipsilateral proximal partial salpingectomy is very rare. High index of suspicion in those cases is of paramount importance. Total salpingectomy should be the gold standard in treating tubal pregnancy.
Competing Interests
There are no competing interests.
| References | ▴Top |
- Baxi A, Kaushal M, Karmalkar H, Sahu P, Kadhi P, Daval B. Successful expectant management of tubal heterotopic pregnancy. J Hum Reprod Sci. 2010;3(2):108-110.
doi pubmed - The management of tubal pregnancy, RCOG Green Top Guidelines No. 21. 2010.
- Tabandeh A, Besharat M. Recurrent ectopic pregnancy in the fallopian tubes. J Clin Diag Research. 2012;6(3):493-494. ISSN-0973-709X.
- Samiei-Sarir B, Diehm C. Recurrent ectopic pregnancy in the tubal remnant after salpingectomy. Case Rep Obstet Gynecol. 2013;2013:753269.
- Storeide O, Veholmen M, Eide M, Bergsjo P, Sandvei R. The incidence of ectopic pregnancy in Hordaland County, Norway 1976-1993. Acta Obstet Gynecol Scand. 1997;76(4):345-349.
doi pubmed - Zuzarte R, Khong CC. Recurrent ectopic pregnancy following ipsilateral partial salpingectomy. Singapore Med J. 2005;46(9):476-478.
pubmed - Fischer S, Keirse MJ. When salpingectomy is not salpingectomy-ipsilateral recurrence of tubal pregnancy. Obstet Gynecol Int. 2009;2009:524864.
- Lau S, Tulandi T. Conservative medical and surgical management of interstitial ectopic pregnancy. Fertil Steril. 1999;72(2):207-215.
doi - Yano T, Ishida H, Kinoshita T. Spontaneous ectopic pregnancy occurring in the remnant tube after ipsilateral salpingectomy: a report of 2 cases. Reprod Med Biol. 2009;8(4):177-179.
doi - Takeda A, Manabe S, Mitsui T, Nakamura H. Spontaneous ectopic pregnancy occurring in the isthmic portion of the remnant tube after ipsilateral adnexectomy: report of two cases. J Obstet Gynaecol Res. 2006;32(2):190-194.
doi pubmed
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Clinical Gynecology and Obstetrics is published by Elmer Press Inc.
